

Though it affects the skin, hidradenitis suppurativa is an inflammatory skin disease, which means people with this condition have irregularities in their immune system.1
There are a number of conditions that have been associated with hidradenitis suppurativa – some of these conditions include:2
Arthritis is known to cause pain and inflammation in the joints, typically worsening with age.3 In Canada, 16.6% of the adult population reports arthritis.4 People living with hidradenitis suppurativa are more likely to have arthritis than the general population.1,2
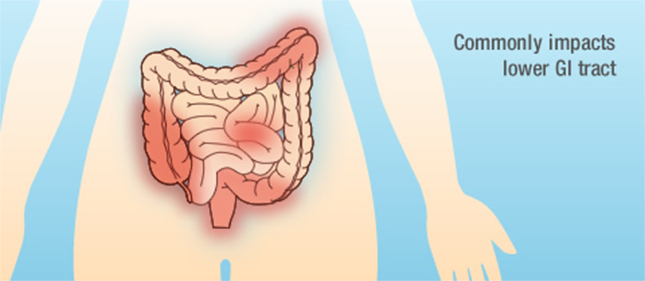
Crohn’s disease is a type of inflammatory bowel disease that causes irritation of the digestive, or gastrointestinal (GI), tract. It most commonly affects the last section of the small intestine (ileum) or the large intestine (colon), but may occur anywhere from the mouth to the end of the rectum. Inflammation can damage sections of the GI tract over time, resulting in additional complications, such as narrowing of the colon.5
Nearly one-fifth of patients living with hidradenitis suppurativa may be affected by Crohn’s disease.1,2
HS has been shown to have a substantial negative effect on the quality of life for people with this skin disease. Evidence suggests that people with HS may also experience depression. Depression is a medical condition that causes a persistent feeling of sadness, loss of interest and hopelessness. The severity of symptoms can vary from person to person. 1,6,7,8,9

People with HS have a higher risk of cancer compared to the general population. Specific cancers reported include cutaneous squamous cell carcinoma, buccal cancer and hepatocellular cancer.1
Severe acne typically involves deeply embedded solid nodules, inflammation and extensive skin damage. Affected areas may become infected, which may lead to scarring if not treated.10,11
Severe acne is associated with hidradenitis suppurativa, though there is the possibility of misdiagnosis of acne in people living with HS.1
Additionally, HS can impact the quality of life of people living with this skin disease.1 If you are living with any of these associated conditions, your dermatologist or health care provider may refer you to another specialist.
Metabolic syndrome describes a group of conditions associated with increased risk of cardiovascular disease. They consist of abdominal obesity, high blood pressure, high blood sugar and abnormal levels of lipids (e.g. cholesterol) in the blood.2
In one study, up to 50% of HS patients had metabolic syndrome, which is higher than in the general population.3
PCOS is a condition in which a woman’s hormones are out of balance.4 Women with HS may have PCOS more frequently than in the general population.
In one study, 38% of women with HS had polycystic ovarian syndrome. The inflammatory skin disease needs to be considered in women who show signs of having PCOS, including irregular period and hirsutism (excessive hair growth in women in uncharacteristic places).5
The open sores and scar tissue cause limited and/or painful movement, especially when the skin disease manifests in the armpits, thighs, groin area or abdomen.
The most common sites where hidradenitis suppurativa manifests also contain many lymph nodes. Scar tissue can interfere with the lymph drainage system, which may result in swelling of the arms, legs or genitals.
The location, drainage and odour of the skin sores — solely or in combination — can be embarrassing and cause reluctance to go out in public, which may contribute to depression.
These wounds can cause severe emotional and physical stress. HS wounds often remain in the inflammatory stage for extended periods of time.
Severe hidradenitis suppurativa may leave rope-like scars, pitted skin or patches of skin that are darker than normal.